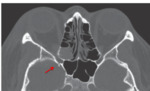
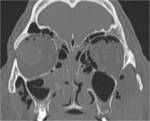
•Computed tomography (CT) is the method of choice for evaluating orbital trauma:
a.
a fast method to perform
b.
readily available
c.
no special need for patient preparation
d.
the eye movement do not degrade the image acquisition
e.no risk if metallic fragment are suspected
• Indications for Imaging in Orbital Trauma are :
* evidence of fracture on clinical examination
* limitation of EOM
* decreased visual acuity in setting of trauma
* severe pain
* inadequate examination due to soft tissue swelling.
•The optimal protocol is thin-sliced CT scan (0.625–1.25 mm) cut through the orbit performed with a helical CT,
then to perform multiplanar reformation.
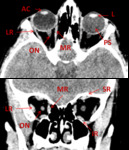
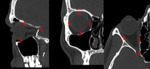
•In general, vertical structures are better seen on axial scans and horizontal structures are better seen on coronal scans :
♦ Axial orientation are best for visualizing most frontal fractures as well as NOE fractures and the zygomatic arches and vertical orbital walls.
♦Coronal orientation was better for the orbital roofs and floors and the pterygoid plates.
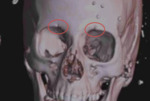
♦The 3D reformation is a useful tool to guide treatment.
It creates an overview picture that may help the surgeon visualize the overall facial architecture.
A.Orbit imaging anatomy
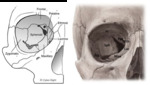
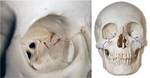
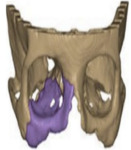
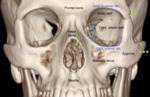
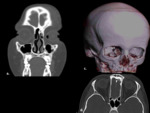
•The orbit is a pyramidal space formed by 7 bones (Fig.1).
•The orbits has the shape of a four-sided pyramid with its axis set from the sagittal plane by an angle of 20°.
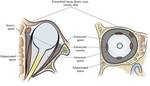
•The globe lies in the anterior orbit.
•The lens divides the globe into (Fig.
2) :
-Anterior chamber : aqueous humor
-Posterior chamber : vitreous humor
•An anatomical characteristic of the orbit is that structures are arranged in groups of 7: there are
⊗7 bones
⊗7 intraorbital muscles
⊗ 7nerves in the orbit
1- The medial wall (Fig 2 ,
3) :
- Rectangular
- Formed by 4 bones :
• Frontal process of the maxilla (forms the medial orbital rim)
• Lacrimal bone
• Orbital plate of the ethmoid
• Lesser wing of the sphenoid
- The medial wall articulates with the roof at the fronto-ethmoid suture (Fig.
4) and it articulates with the the floor at the maxillo-ethmoid suture.
2- The orbital floor :
It is the roof of the maxillary sinus (Fig 6).
In its posterolateral 2/3 ,
the floor is separated from the lateral wall by the inferior orbital fissure through which the maxillary division of the trigeminal nerve enters the orbit.
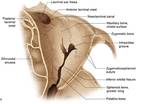
The infraorbital groove(Fig 7): location of infraorbital nerve that supplies sensation to check and ipsilateral upper alveolus and teeth.
3- The lateral wall :
•It is the thickest of the orbital walls
• Lateral orbital wall is formed anteriorly by the zygoma and posteriorly by sphenoid (Fig 8).
•Zygomatic bone consititues the midfacial prominence which make it highly susceptible to trauma.
• It forms the lateral portion of the inferior orbital rim,
as well as the lateral rim and lateral wall of the orbit
• It is separated from the floor by the inferior orbital fissure and from the roof by the superior orbital fissure (posteriorly) and the frontosphenoid suture (Fig.
9).
•In its posterior part,
the greater wing of sphenoid is interposed between the middle cranial fossa and the orbit.
4- The orbital roof ( Fig 10) :
It is formed by the frontal bone with a minimal contribution =>from the lesser wing of sphenoid.
=>It forms the floor of the anterior cranial fossa.
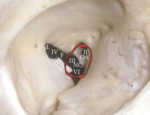
5- The orbital apex :
•Includes the area lateral to the optic canal through which cranial nerves III, IV, V, and VI pass to enter the orbit.
•The optical canal is considered part of the superior orbital fissure(Fig.11).
• When pressure from an injury causes dysfunction in these nerves, it is
called superior orbital fissure syndrome, which requires urgent surgical intervention.
•The supra orbital notchis part of the superior orbital rim (Fig.12).
•The supraorbital nerve passes through the supraorbital notch prior to dividing into superficial and deep components that provide sensory innervation to the ipsilateral forehead.
6- the intraorbital posterior structure :
•Seven are the intraorbital muscles: levator palpebrae,
superior,
inferior,
lateral,
and medial rectus,
and superior and inferior oblique muscles.
•Only the inferior oblique muscle is attached to the medial orbital wall.
•The four recti and the superior oblique muscles attach along the orbital apex in and around a common annular tendon or fibrous ring,
the annulus of Zinn.
•The annulus inserts along the orbital apex,
encircling the orbital opening of the optic canal and the central part of the superior orbital fissure .
•Veins and lymphatic lie within the orbital fat of the muscle cone centrally.
•The optic nerve sheath passes from the posterior globe to the brain.It is an extension of the dura mater and contains the ophthalmic artery,
the optic nerve,
and small veins.
•The orbital nerves are 7.
With the exception of the optic nerve which transits through the optic canal,
all others pass along the superior orbital fissure(Fig .
13).
B- Systematic approach:
This is a systematic approach to assist rapid evaluation of the orbit using a comprehensive list .
When evaluating a patient with an orbital injury,
the radiologist should do the following:
1.
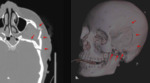
evaluate for external soft tissue changes
2.
evaluate anterior chamber
3.
evaluate position of the lens
4.
evaluate globe including posterior segment
5.
evaluate bony orbit for fractures
6.
evaluate for foreign bodies
7.
evaluate vessels and optic nerve
8.
always look for associated intracranial injury to CNS
I.
Evaluate for external soft tissue changes:
The surgical spaces of the orbit are ( Fig 14):

Table 2: The surgical spaces of the orbit
References: Radiology department Sahloul University hospital
II.
Evaluate the anterior chamber.
Increased attenuation suggests a hyphema.Decreased depth suggests either a corneal laceration or anteriorsubluxation of the lens.
Increased depth is associated with open-globe injuries.
III.
Evaluate the position of the lens:
The lens may be displaced,
either anteriorly or posteriorly,
and it may be either completely or partially dislocated (Fig.15).
IV. Evaluate the Bones Anterior chamber
•Evaluate the bony fractures
• Note any herniations of orbital contents
•Pay particular attention to the orbital apex
•Fractures involving orbit may be classified according to the pattern of involvement of :
I.walls of the orbit
II.rim of the orbit orbital fractures associated with fractures involving other facial bones.

Table 3: Classification of orbital fractures
References: Radiology department Sahloul University hospital
•Blow out and Blow in fractures
•Orbital floor,
medial wall,
or roof can be involved.
•This type of fracture can be further classified into:
=>Trap door type of fracture – due to low velocity injuries
=>Medial blow out fractures – due to intermediate velocity injuries
=>Lateral blow out fractures – due to high velocity injuries
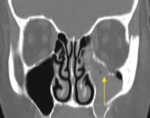
a.i.Orbital floor fracture (Fig.16,
17):
Orbital floor fractures can occur isolated or associated with :
•Le Fort II fractures (orbital floor fractures) .
•NOE fractures (medial orbital wall fractures).
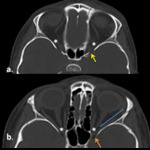
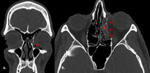
a.ii.
Fracture medial wall of orbit:
•Isolated fractures involving the medial wall of orbit is rather rare.
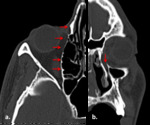
•Most commonly they form a component of naso orbito ethmoidal fractures and hence the name (NOE) (Fig.18).
•Medial orbital wall trauma is strongly related with diploplia due to the mechanical entrapment of the medial rectus muscle .
•This fracture is difficult to diagnose without the aid of CT imaging.
• On CT it is recognized by displacement of the muscle into the fracture site, with or without bone displacement.
• Subtle medial wall fractures can be detected by comparing the distance from the midline to the medial wall on the injured and uninjured sides.
•The fractured side will often show a decreased distance in comparison to the unaffected side.
• 3D reconstruction is currently used for selecting and fashioning the desired implant in the perioperative period,
and even usingmodels covered in sterile plastic intraoperatively to mold synthetic implants.
•The application of this approach allows the surgeon to repeatedly go between the defect and the model in real time to allow for minute refinements in the bone graft before fixation.
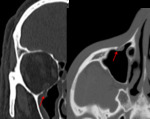
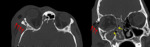
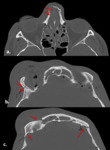
b. Blow out fracture :
•They are produced by direct impact on the orbit by an object larger than its circumference.
• This kind of lesion is more prevalent in the orbital floor.
•It produces,
most commonly, a floor or medial wall fracture with fragment displacement out of the orbit toward the interior of the maxillary sinus (Fig.
19).

Table 1: classification of the blow out fractures
References: Radiology department Sahloul University hospital
These fractures are differentiated into pure or impure type depending on the involvement of the orbital rim.
b.i Orbito-zygomatic fracture (Fig.20):
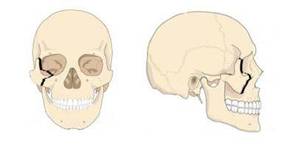
Fig. 28
References: http://www.chirurgiemaxillofaciale-albi.com
It may involve:
•Lateral orbital wall
•Infraorbital rim
•zygomatic Arch
•Zygomatic buttress
c. Complex fracture:
=>Zygomaticomaxillary Complex ( ZMC) Fractures:
•Typically occur across the three buttress-related sutures,
leading to the term (Fig.
21).
•A displaced ZMC fracture is a quadripod fracture .
d.
Blow-In fracture:
•Blow in fractures are less frequent.
•They are produced by a small object impact that produces a fracture with displacement of fragments into the orbit.
•They result from direct injury to the para-nasal sinus region with centrifugal displacement of bone fragments.
• These fractures are extensions of supra-orbital rim fractures.
•Isolated non displaced fractures involving roof of frontal bone are uncommun in adults.
•In children younger than 7 years,
in whom the frontal sinus is not yet pneumatized frontal fractures affect the orbital roof almost exclusively,
but they also may extend to the frontal bone (Fig.22).
=> NOE fractures (Fig.
20,
23,
24):
•NOE fractures are distinguished from simple nasal fractures by posterior disruption of the medial canthal region,
the ethmoids,
and the medial orbital walls.
•If there is bilateral comminution and displacement in this region,
the nasofrontal ducts that drain the frontal sinus are also likely disrupted .
•Radiologic description should comment on the degree of comminution of the medial vertical maxillary buttress,
specifically in the region of the lacrimal fossa,
where the medial canthus attaches.
• The distance between the two lacrimal fossae in the coronal plane is also important,
as it will alert the surgeon to the need for a medial canthoplasty.
d.
Orbital apex fractures (Fig.25):
=>These fractures should be identified early
=>Potential threat to neurovascular structures at superior orbital fissure and optic canal.
=>Optic canal injuries can lead to traumatic optic neuropathy .
IV.
Fractures involving orbital rim / along with internal orbital skeleton :
These fractures may be subclassified into:
=>Inferior rim fracture
=>Superior rim fracture
=>Lateral rim fracture
=>Rim fracture in association with fractures involving internal orbital skeleton
V.
Fractures of orbit associated with other fractures of facial skeleton. (Fig.26):
These include:
=>zygomatico maxillary fracture (ZMF)
=>Naso-orbito-ethmoid fracture (NOE)
=>Frontal sinus fracture
=>Lefort II
=>Lefort III
VI.
evaluate for foreign bodies:
•Evaluate for radiopaque or radiolucent foreign bodies
• Remember that wooden foreign bodies can mimic air on CT scans
VII.
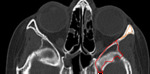
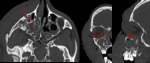
evaluate vessels and optic nerve (Fig.27)
•Try to localize the fluid collections,
remembering the characteristic shape of fluid collections in a retinal or choroidal detachment Evaluate the ophthalmic veins and the optic nerve complex.
•The presence of posttraumatic diplopia associated with proptosis and chemosis suggests a diagnosis of carotid cavernous fistula.
• On unenhanced CT scans of the orbit,
a dilated superior ophthalmic
vein is usually seen,
isolated or in association to other signs of carotid cavernous fistula (cavernous sinus thrombosis,
venous varix,
Graves disease).
•The optic nerve may be transected,
particularly in penetrating traumas.
•In blunt traumas,
the key area to evaluate is the orbital apex.
• Most commonly,
a definitive fracture is not found.
In these cases,
the optic nerve or its vascular supply is torn,
thrombosed,
or compressed
VIII.
always look for associated intracranial injury to CNS:
• Look for bleeds or abnormal fluid collections